Introduction
In the realm of life sciences, the advancement of medical knowledge and the development of novel therapies heavily rely on the execution of meticulously designed clinical trials.
Clinical research plays a pivotal role in ensuring the safety and efficacy of pharmaceuticals, medical devices, and treatment methodologies. However, orchestrating these trials efficiently and effectively demands robust infrastructure and seamless coordination among researchers, sponsors, and regulatory authorities.
In this context, Clinical Trial Management Systems (CTMS) have emerged as indispensable tools, aiming to streamline trial operations and enhance research outcomes. Nevertheless, a critical inquiry arises:
Do CTMS truly meet the multifaceted needs of researchers?
This article delves into this question, scrutinising the functionality, usability, and overall efficacy of CTMS from the perspective of life science professionals.
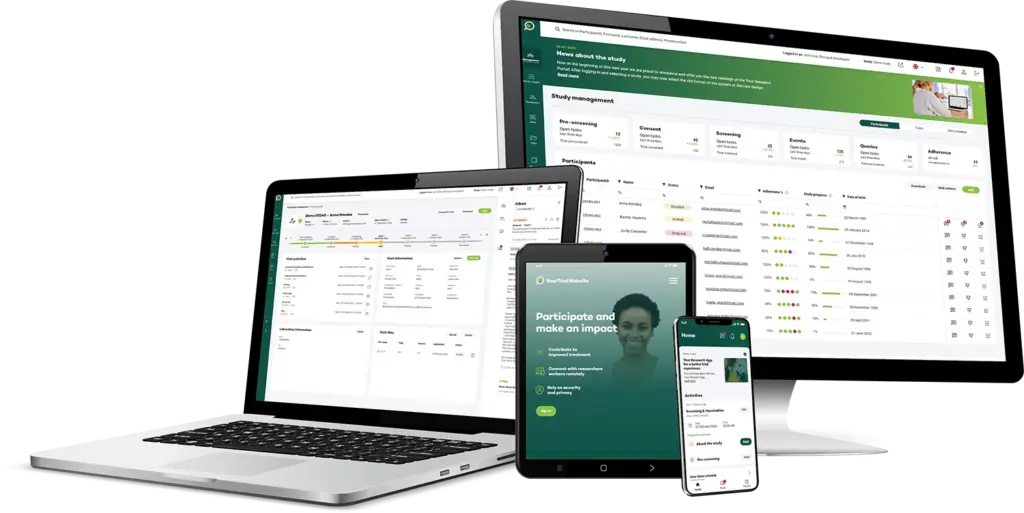
Functionality of CTMS
At its core, a CTMS is designed to facilitate the planning, execution, and monitoring of clinical trials. It encompasses a wide array of functionalities, including subject recruitment, protocol management, data collection, regulatory compliance, and financial tracking. Proponents argue that CTMS significantly expedites trial timelines, improves data accuracy, and ensures compliance with regulatory standards.
However, the reality often diverges from these promises. Many researchers encounter challenges in navigating the complexities of CTMS platforms, citing issues such as unintuitive interfaces, limited customisation options, and inadequate integration with other research tools.
Moreover, the one-size-fits-all approach of certain CTMS solutions may not align with the diverse needs and workflows of researchers across different therapeutic areas and study designs.
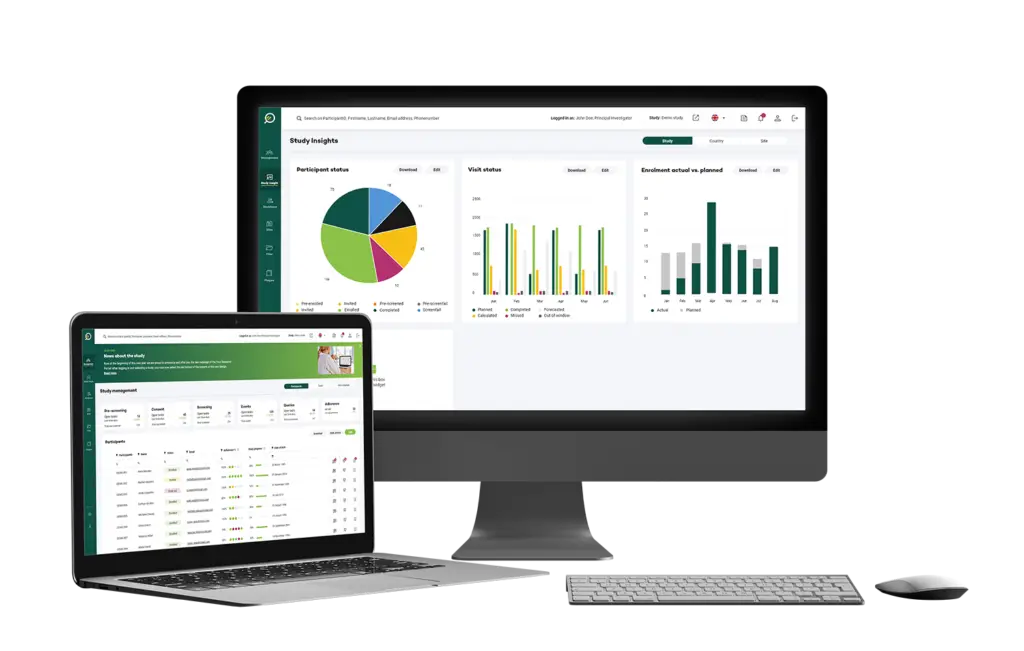
Usability and User Experience
The usability of CTMS emerges as a pivotal determinant of its effectiveness in meeting researcher needs. While some platforms boast sophisticated features, their usability remains a major pain point for end-users. Cumbersome interfaces, convoluted workflows, and steep learning curves can impede researchers’ productivity and hinder their ability to focus on scientific inquiry.
A study by Thoma et al. (2019) highlighted the significance of user-centered design principles in enhancing the usability of CTMS. By incorporating feedback from end-users and prioritizing intuitive interface design, developers can mitigate usability challenges and foster greater acceptance of CTMS within the research community.
Additionally, the accessibility of CTMS across different devices and operating systems is crucial for enabling seamless collaboration among geographically dispersed research teams.

Integration and Interoperability
Another critical aspect in evaluating the efficacy of CTMS is its integration capabilities with other research infrastructure and data systems. In the era of big data and interconnected research ecosystems, siloed platforms pose significant barriers to data sharing and collaboration.
Researchers often grapple with the fragmented nature of information across disparate systems, leading to inefficiencies in data management and analysis.
Therefore, CTMS must exhibit robust interoperability with Electronic Health Records (EHRs), Laboratory Information Management Systems (LIMS), and other relevant databases.
The adoption of standardized data formats and Application Programming Interfaces (APIs) facilitates seamless data exchange and enhances the interoperability of CTMS with external platforms.
Moreover, interoperable CTMS empower researchers to leverage advanced analytics and artificial intelligence algorithms for deriving actionable insights from clinical trial data.

Conclusion
While Clinical Trial Management Systems hold immense potential in streamlining research operations and driving innovation in the life sciences sector, their efficacy in meeting researcher needs remains contingent upon various factors. From functionality and usability to integration and interoperability, CTMS must align with the evolving requirements of the research community to fulfil their intended purpose. As stakeholders continue to navigate the rapidly changing landscape of clinical research, collaboration between developers, researchers, and regulatory agencies is imperative for refining existing CTMS solutions and fostering a culture of innovation in clinical trial management.
References:
Park Y, Yoon Y, Koo H, Yoo S, Choi C, Beck S, Kim T
Utilization of a Clinical Trial Management System for the Whole Clinical Trial Process as an Integrated Database: System Development J Med Internet Res 2018;20(4):e103 URL: https://www.jmir.org/2018/4/e103
DOI: 10.2196/jmir.9312
Fegan GW, Lang TA (2008) Could an Open-Source Clinical Trial Data-Management System Be What We Have All Been Looking For? PLoS Med 5(3): e6. https://doi.org/10.1371/journal.pmed.0050006
Zhengwu, Lu, Jing, SuPY – 2010/06/01 Clinical data management: Current status, challenges, and future directions from industry perspectives 10.2147/OAJCT.S8172 Open Access Journal of Clinical Trials



